Revision Hip Surgery
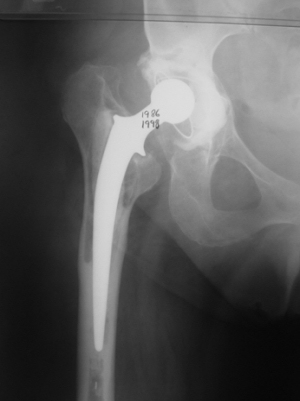
Information about Hip Revision Surgery
Hip revision surgery involves the repair of an artificial hip joint that has been damaged or loosened over time or as the result of infection. The use of artificial hip implants has become quite widespread in recent years. They can be extremely effective in improving hip joints that have been severely damaged by injury or arthritis.
In hip replacement surgery the diseased portions of the hipbones are cut away and replaced with a two-part prosthesis, or artificial hip joint. With revision surgery the original prosthesis is removed and replaced with a new one. Sometimes this is a long process involving more than one surgical procedure, and is certainly more taxing than the original replacement surgery.
The human hip, is a ball and socket joint, in which the ball of one bone (the femur, or bone of the upper leg) fits into the socket of another (the pelvic bone). As a free-moving joint in the body, the normal hip can move backwards and forwards, from side-to-side, and can perform twisting motions.
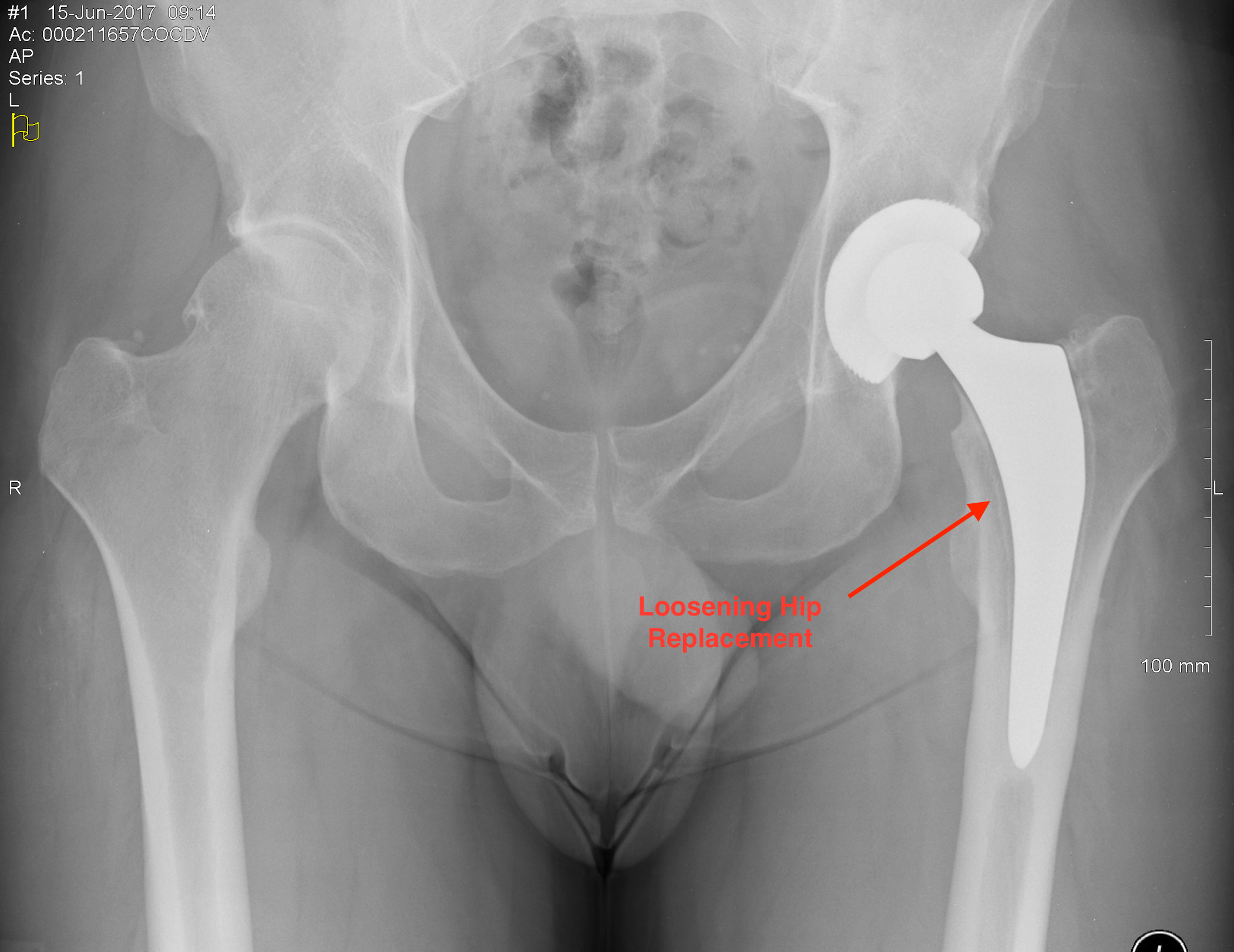
Loosening Hip Replacement
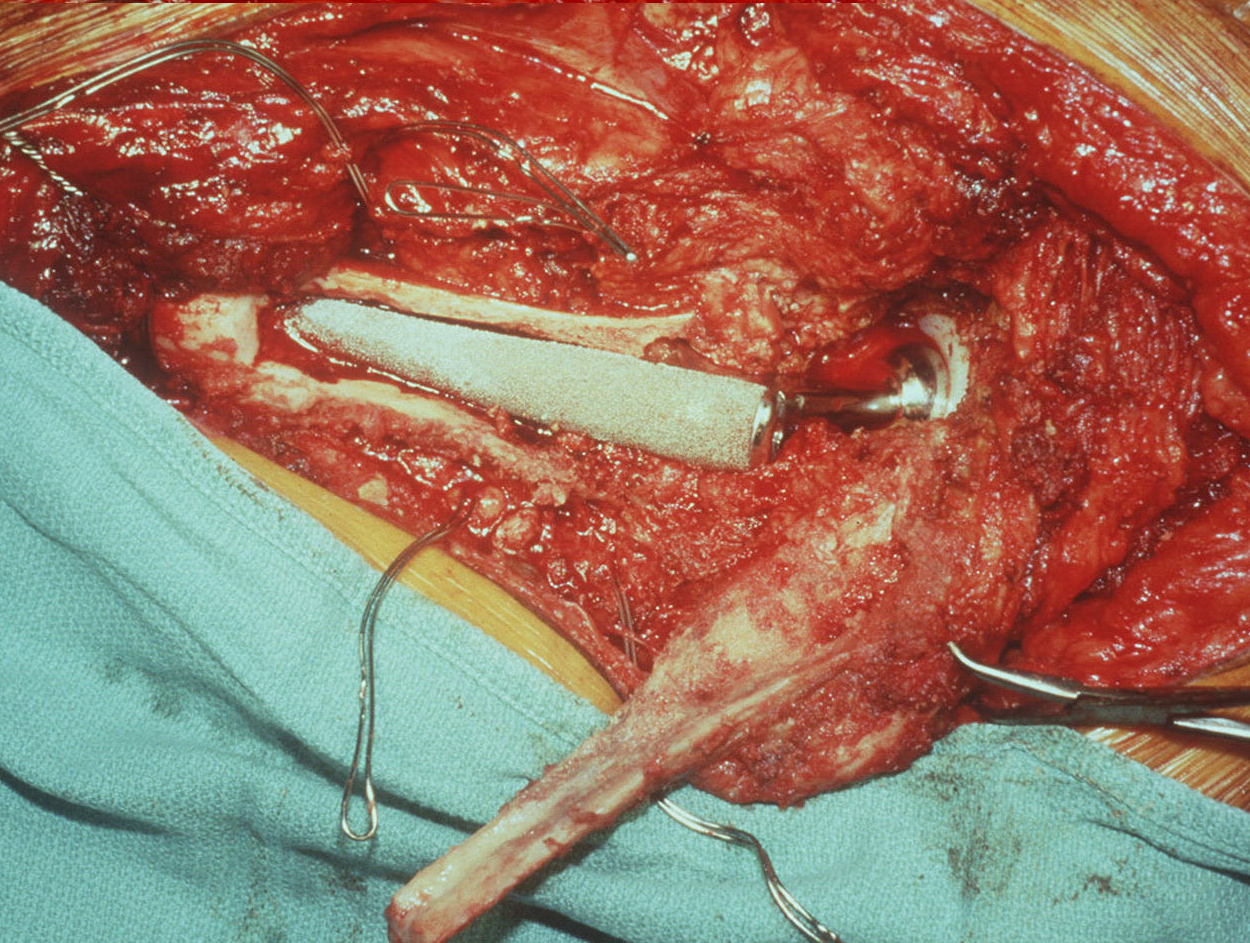
Implantion of a Hip Replacement
Reasons For Having Revision Hip Surgery?
Artificial joints do not last forever, and many show signs of loosening after a period of 10-15 years. When an artificial joint is no longer securely attached to the bone, it is commonly because the bone absorbs next to the prosthesis; thus, new abnormal motion occurs, resulting in pain on weight bearing. Revision surgery is an attempt to correct the problem in order to get the hip back to a condition where it can function normally.
Patients who have had an artificial joint implanted in their hip are usually people aged 55 or older who developed severe and debilitating arthritis in the hip joint. After a period of 10-15 years, the artificial joint may no longer fit securely. The pressure brought to bear on the hip, a major weight-bearing joint, eventually loosens the prosthesis and compromises its effectiveness.
Sometimes revision surgery is needed because infection has spread to surrounding tissue in the joint. When infected, the muscle, tendon, and ligament tissue in the joint can become damaged, losing elasticity and strength. Infection damages the bone, destroying bone stock that was present in the original surgery. If infection has developed in the hip joint, more than one revision surgery may be required. A first procedure may be needed to take out the old prosthesis scar tissue and then infuse the joint with antibiotics. At a later date, when the hip is cured of infection, surgery for a new prosthesis can be performed.
Pain relief is the most reliable potential benefit and often the major reason for hip revision surgery. For most people, a hip revision also offers better movement, strength, and coordination of the torso and leg. When a prosthesis is successfully replaced, the patient may experience another long period of time with relatively few problems in the hip.
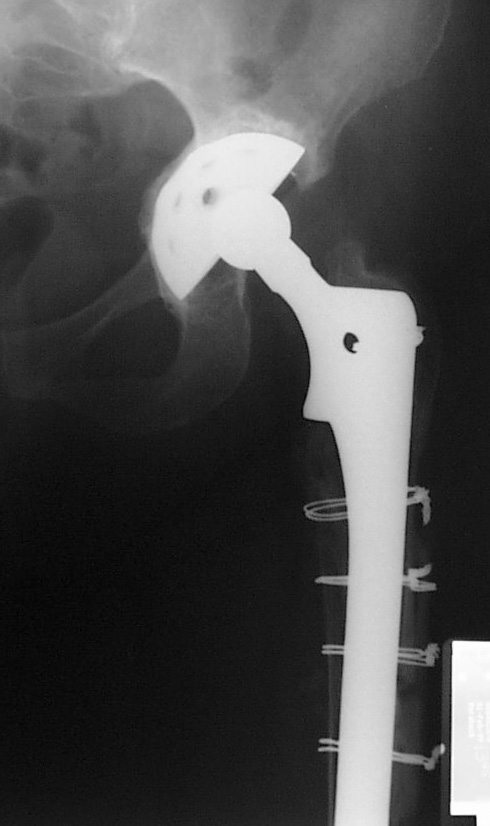
X-ray of a Revision Hip Replacement
Surgical Procedure for Hip Revision Surgery?
Surgery to repair or replace a loosened prosthetic hip joint is usually more difficult than the initial hip replacement. There may be less bone for the surgeon to work with, or more bone grafting may be needed to secure the second implant. The recovery period for revision surgery is usually longer as well, in part because the patient is older and often in weaker general health.
In preoperative evaluations, the surgeon tries to determine the exact surgical method to be used, taking into account the particulars of your individual case. He or she decides on the type and size of the new prosthesis. An effort is made to determine whether you will need additional bone grafts or other procedures to improve the quality of bone and tissue in the joint. If the joint has been damaged by infection, the surgeon will explain the need for multiple surgeries.
Surgery is performed by means of open incision. Commonly, these difficult operations take several hours. The old prosthesis is removed and, if possible during the first surgical procedure, replaced with a new one.
Rehabilitation After Hip Revision Surgery?
A physiotherapist will help you begin walking, first with a frame and then independently.
Major surgery like hip joint revision requires a period of adjustment. Take it easy during this time, trying to focus on the healing process and in gradual, practical improvements to your general condition. It is important to exercise your legs, as this reduces swelling. Elevate your legs above your heart whenever you are at rest.
After hip revision surgery, a patient will only get around with a walker. Normal everyday things like getting into a car or walking up steps will be difficult. It won’t be long before a patient can put weight on the injured leg.
Having already taken part in physical therapy after the initial hip replacement surgery, a patient will be familiar with the physical therapy.
After about a month, a physician will take x-rays of the leg to monitor its healing. After about six months, patients with hip revision surgery will be able to walk without a limp, and the hip should no longer cause pain.
People who have hip revision surgery must be particularly cautious about infection. After the procedure, it is wise to always tell your dentist or physician that you have an artificial joint.
Having a large metal implant in your hip may sometimes set off metal detectors in an airport or at a public event. Just as before the revision surgery, you should carry a card identifying you as a patient with an artificial implant.
Possible Complications of Hip Revision Surgery?
Hip revision surgery is usually an elective procedure. The original artificial joint should be replaced with one of the high-quality prostheses currently available.
There may occasionally be unforeseen complications associated with anesthesia, including respiratory or cardiac malfunction. The procedure may be complicated by infection, injury to nerves and blood vessels, fracture, weakness, stiffness or instability of the joint, pain, or the need for additional surgeries.
Patients who may be at increased risk for complications include those who are immunocompromised in some way, such as patients with severe rheumatoid arthritis or systemic lupus. Those with disease, drug, or radiation-induced immunosuppression are also at increased risk, as are patients with insulin-dependent (type 1) diabetes, malnourishment, hemophilia, or those who have had previous prosthetic joint infections.
Many variables affect the ultimate success of hip revision surgery, including the strength of the patient’s bone and musculature, his or her general health (including mental and emotional health) and lifestyle. Commitment to rehabilitation is a key part of the process, as improvement to the hip joint is determined not only by surgery but also by rehabilitative effort.
If you would like any further information about arranging a revision hip replacement in central London with Mr. Jig Patel FRCS please contact us to arrange a consultation.
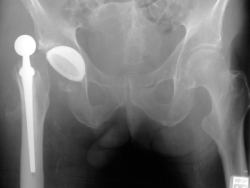
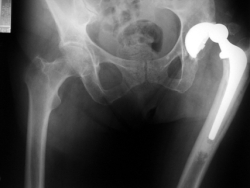
The hip may dislocate if components have been malpositioned; the hip has been put into an extreme position, particularly early after surgery; and if the muscle control of the hip is poor. Thankfully, dislocation should be a rare complication, but can occur in 3% of cases.
